Healthcare Inbox
Redesign
Helping clinicians triage and act on critical information faster
ROLE
Senior UX Designer
TIMELINE
12 Weeks (Research & Design)
TEAM
1 PM, 5 Engineers, 1 UXD
Case study overview (video summary)
Accessible video summary of the case study, offering an alternate format to the written content for easier consumption.
.png)
.png)


EXECUTIVE SUMMARY
Clinicians depend on the EHR inbox to manage critical patient information, but the legacy experience was cluttered, poorly prioritised, and disrupted clinical workflows.
As Lead Product Designer, I guided the redesign end to end — from research to launch — partnering with clinicians, product, and engineering to create a triage-first inbox. The goal was to help providers see what matters first, act confidently, and resolve items quickly without unnecessary navigation.
4.27/5
Average Satisfaction Score
Clinicians were happier and satisfied than before
15%
Faster to first action
In field installation confidence
12%
Fewer clicks to common inbox actions
On excel for reporting and operational source of truth
"This redesign was not a UI polish — it changed how clinicians interact with critical patient communication"
The World Before
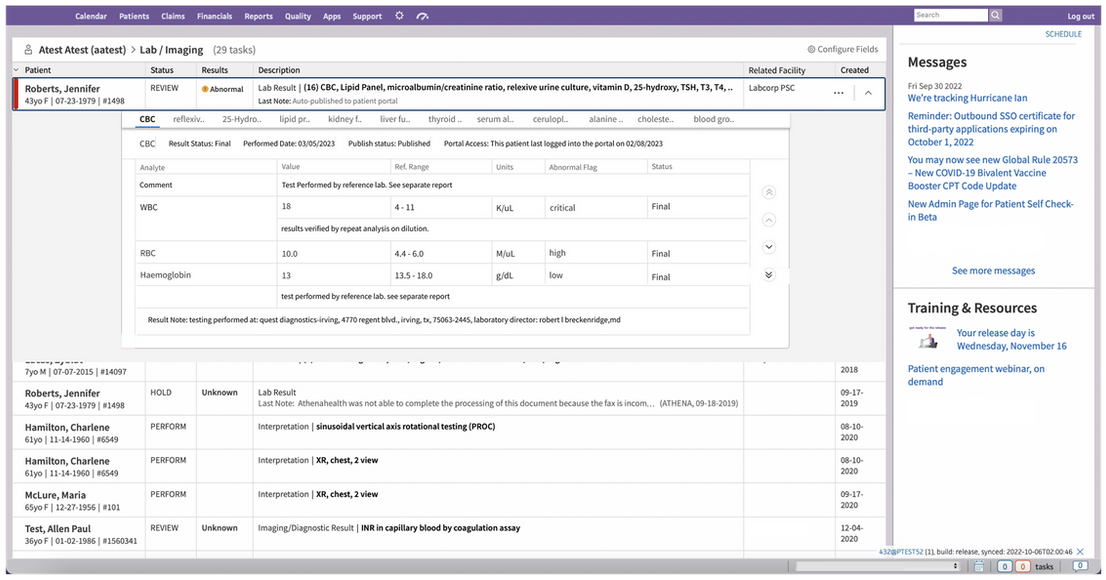
In the legacy EHR, the inbox looked like a laundry list — all messages blended together regardless of urgency or context. Clinicians had to open each message separately, wait for a slow detail screen to load, and then decide what to do next. Each review was its own workflow detour.
Lab results, imaging reports, medication alerts, and other care items were all mixed together, with no clear indication of urgency or context. Clinicians knew something important might be in there — but the system didn’t help them find it quickly.

The old inbox made clinicians work to understand what to prioritise, wasting precious time.
Understanding the Work Before Designing Anything
To redesign effectively, we needed to step into clinicians’ shoes.
We interviewed and shadowed a large mix of users — from physicians and registered nurses to care coordinators — across outpatient and inpatient settings. We walked their workflows, observed how they interacted with the inbox in real moments, and logged pain points such as:
Lab results buried at the bottom of a list
Frequent context switching between inbox and chart
Critical items taking too long to review
Frustration at having to open every message just to know its content
Quantitatively, clinician satisfaction with lab result review hovered under 40%, and scanning long lists of unread items was a dominant early pain point.
Designing a healthcare inbox is about supporting high-stakes, interruption-heavy clinical work.
Where Things Broke
We learned that clinicians were already trying to cope with the old tool: scanning lists rapidly, opening multiple screens, returning to lists, and losing their place.
But the system frequently broke these coping strategies. Slow loading details, no triage cues, and no prioritisation forced clinicians to do mental filtering themselves — all while juggling patient care.
This led to:
-
Longer time to first meaningful action
-
Higher Cognitive Load
-
Greater risks of missing critical results
-
Frustration & Lower Satisfaction
The tool didn’t just slow them down — it disrupted clinical reasoning, which is where real risk lies.
Guiding the Team Through Ambiguity
At the start, there was ambiguity on what “better” meant in a healthcare inbox. Some stakeholders thought cleaner visuals would help; others pushed for more filtering, while engineering cautioned about performance and legacy system constraints.
My role was to slow the team down and avoid over indexing on Stakeholder suggestions, I guided the team to:
Map the full workflow end-to-end
Understand the different mental models of clinicians, their actions and why
Identify where mistakes actually occurred
I repeatedly brought the conversation back to one question:
"What is the user trying to accomplish (JTBD) & What decisions they making"
That question shifted our focus from “make it prettier” to “reduce cognitive effort at the moment of clinical decision making.”
We held working sessions with clinicians, ran virtual ride-alongs, and dogfooded the inbox ourselves. This revealed that priority cues, scannability, and quick context access were far more valuable than decorative detail.
Design ambiguity resolves when we understand users' mental model on the job
The Strategic Shift
Rather than designing a traditional filtered list, we made three strategic decisions:
1. TRIAGE AT A GLANCE
Urgency and Intent must be visible without opening each item.
2. ACT WITH CONTEXT
Key results and actions should be surfaced inline, not buried behind slow detail screens.
3. RESOLVE AND MOVE ON
Once resolved, the item should exit the inbox cleanly to reduce noise.
This shifted the inbox from being an archive of messages to a workflow engine for action.
Prioritisation, not aesthetics, was the strategic north star.
Leading Through Tensions and Trade-offs
This project had natural tensions:
Design vs. Familiarity: Clinicians trusted the old scanning method even though it was inefficient. Changing defaults met initial resistance.
Performance vs. Density: Healthcare professionals wanted dense information; engineering reminded us of performance limits with legacy servers.
Change vs. Safety: In healthcare, every design change must preserve clinical safety and avoid unintended risk.
Our approach was evidence-led. We backed proposals with real clinician statements, observation data, and task success metrics.
I wasn’t always right. A proposed default sort order initially increased cognitive load for power users, and that taught me the importance of gradual rollouts and opt-in preferences in clinical tools.
In healthcare, leadership is prioritising safety over novelty
What We Ultimately Built
Desktop Experience
The desktop inbox was the primary triage workspace, surfacing urgency, priority, and key results inline to enable fast scanning, action, and resolution without leaving the list.
Urgency and priority tags visible in the list
Quick actions (acknowledge, delegate) without navigation
Scannable high-density list with visual cues
Open results without leaving the list
Mobile/Responsive Interaction
A workflow that supports clinicians on the go, enabling quick scans of results without losing context.
The mobile app acted as a companion for clinicians on the go, surfacing critical information for quick awareness, acknowledgement, and follow-up while maintaining continuity with desktop workflows.
This is about as tight as it gets without losing meaning.
Clinicians spend less time looking for what matters and more time acting on it.
Validation & Testing
We conducted two rounds of moderated usability tests with clinicians (physicians, nurses, care coordinators) across outpatient and inpatient contexts. The results were strong
1. Task Success Rate: increased from ~68% to 89%
2. Average Triage time: reduced from 4.2 mins to 3.1 mins
3. User Feedback: "It gives me my lunch break back"
Testing confirmed that scannability + context beats traditional detail screens.
What I Learned
This project reinforced that:
01
Defaults in healthcare act as clinical decisions and must prioritise safety and clarity.
03
Designing for interruption and fast re-entry matters more than optimising for linear task flows.
02
High information density works when hierarchy and prioritisation is clear and consistent.
04
In safety critical systems, clarity and predictability outperforms clever interactions every single time
In clinical systems, UX decisions directly influence safety.
What I Would Do Differently
I would involve compliance and clinical governance partners earlier in the design process. While we aligned successfully later, earlier involvement would have accelerated decision-making around safety-critical trade-offs.
I would also plan more deliberately for in-context onboarding during rollout.